Table of Contents
Understanding Hormonal Acne
At NSS Dermatology in Midtown Manhattan, we frequently encounter patients seeking effective hormonal acne treatment for persistent breakouts that disrupt their confidence and daily lives. According to the American Academy of Dermatology, adult acne affects approximately 15-20% of women, often driven by hormonal imbalances rather than the typical teenage oil overproduction. These hormone-related breakouts tend to flare up in predictable patterns, distinguishing them from other acne types and highlighting the need for targeted management.
Hormonal acne arises from fluctuations in hormones like androgens, which stimulate excess oil production and clog pores, leading to inflammation. Common triggers include the menstrual cycle, where surges occur before periods; pregnancy, with shifting estrogen and progesterone levels; and postpartum changes that can exacerbate oiliness even after delivery. Unlike the widespread pimples of adolescence, this form persists into adulthood, often linked to internal factors such as polycystic ovary syndrome or stress-induced cortisol spikes, as outlined in AAD guidelines on acne causes. Our board-certified dermatologists emphasize that recognizing these patterns is crucial for developing personalized strategies.
Typically, hormonal acne manifests as deep, painful cysts and nodules along the jawline, chin, and lower face, creating tender, inflamed areas that heal slowly and may scar. These appear more cyclically than randomly, reflecting the body’s internal hormonal clock.
While lifestyle adjustments like balanced diets and stress reduction support skin health, professional evaluation remains essential. At NSS Dermatology, we offer comprehensive assessments to tailor options, including medications and therapies, ensuring evidence-based care for optimal results. Understanding these fundamentals paves the way for the effective management strategies explored in the following sections.
Fundamentals of Hormonal Acne
At NSS Dermatology, we frequently encounter patients seeking clarity on skin concerns that disrupt their daily lives. Hormonal acne represents a specific type of acne driven by fluctuations in hormones, particularly androgens, which stimulate oil glands to produce excess sebum. This leads to clogged pores and subsequent inflammation, often manifesting as deep, painful cysts rather than surface-level blemishes. Unlike typical teenage acne, hormonal acne tends to persist into adulthood, affecting areas influenced by hormone-sensitive zones such as the jawline, chin, and lower cheeks.
Identifying hormonal acne involves recognizing its distinct characteristics. These endocrine-triggered pimples appear as large, tender nodules or cysts that develop beneath the skin, creating swelling and discomfort. Common symptoms include:
- Deep, cystic lesions along the lower face
- Persistent redness and inflammation
- Flares that align with hormonal shifts, such as cycle-linked eruptions before menstruation
Pre-period flares often result from rising progesterone levels, which amplify oil production in the days leading up to menstruation. According to the American Academy of Dermatology, hormonal imbalances can exacerbate this, with conditions like polycystic ovary syndrome contributing through elevated androgen levels. Post-pregnancy, many women experience ongoing breakouts due to sudden drops in estrogen, prolonging the condition beyond the typical resolution period. We at NSS Dermatology emphasize that while these patterns provide clues, accurate identification requires professional evaluation to rule out other factors.
Understanding demographics highlights its prevalence. Hormonal acne commonly affects women aged 20 to 40, with the AAD reporting that up to 50% of women in this group experience adult acne linked to hormonal causes. Stress, family history, and even certain medications can intensify these issues, underscoring the need for tailored approaches. For instance, options like birth control for acne or spironolactone for acne address underlying mechanisms by balancing hormones, but only under medical supervision.
Distinguishing hormonal acne from other types is crucial for effective management. The following table compares key characteristics to aid in self-awareness:
| Characteristic | Hormonal Acne | Bacterial Acne | Comedonal Acne |
|---|---|---|---|
| Triggers | Hormone fluctuations (e.g., menstrual cycle) | Androgen surges, PCOS, pregnancy | Propionibacterium overgrowth |
| Appearance | Deep cysts on jawline/chin | Painful, inflammatory nodules | Pustules with pus |
This comparison, informed by AAD guidelines on adult and stubborn acne, illustrates how hormonal acne differs in its deeper, more inflammatory nature compared to bacterial weight or comedonal clogs. Recognizing these distinctions empowers individuals to seek targeted care, potentially leading to adult acne treatment options that address root causes rather than surface symptoms. At our Midtown Manhattan practice, we guide patients through such assessments to develop personalized plans.
Building on this foundation, proper recognition of hormonal patterns paves the way for exploring deeper mechanisms and potential hormonal acne treatment strategies. We recommend consulting a dermatologist for any persistent concerns, as self-diagnosis can overlook underlying health issues like PCOS.
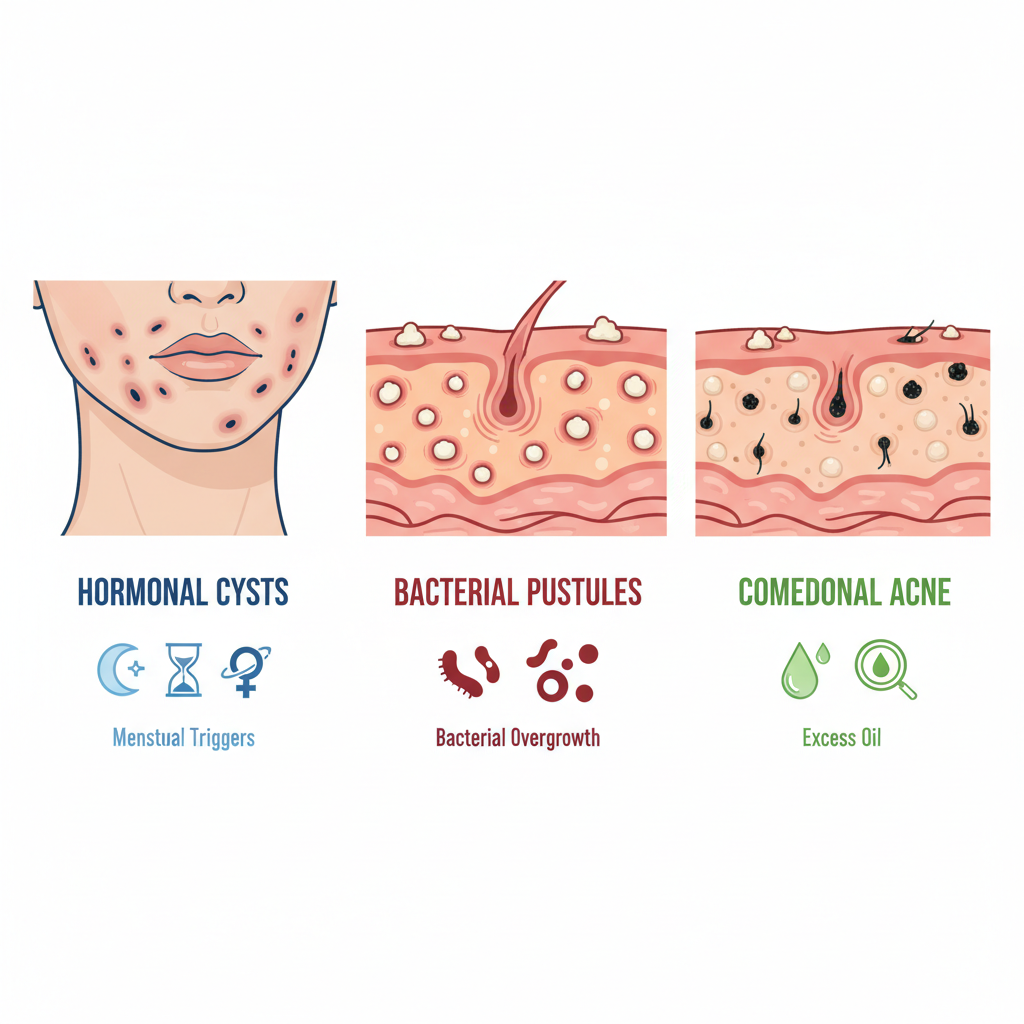
Comparison of hormonal vs. bacterial and comedonal acne types
Hormones act like wave patterns in the body, surging and receding to influence skin health. When these waves become imbalanced, they trigger cycles of irritation that demand attentive care. Our team at NSS Dermatology supports patients in navigating these fluctuations with evidence-based insights and compassionate guidance.
Deep Dive into Hormonal Mechanisms
Our team at NSS Dermatology often sees patients grappling with acne that seems tied to life stages and cycles. Understanding the hormonal mechanisms behind this condition provides crucial insights into why breakouts occur and how targeted interventions can help. Hormones act as conductors in the body’s symphony, directing oil production and inflammation that can lead to acne. By exploring these biological processes, we empower patients to recognize patterns and seek appropriate care, such as hormonal acne treatment options tailored to their needs.
Hormonal Fluctuations and Acne Triggers
Hormonal acne arises primarily from fluctuations in key hormones that influence sebum production in the skin’s sebaceous glands. Androgens, such as testosterone, play a central role by stimulating these glands to produce more oil, which can clog pores and foster bacterial growth. According to insights from the American Academy of Dermatology, hormones contribute significantly to acne in adults, particularly women, where androgen levels can surge during specific physiological changes. For instance, in the menstrual cycle, rising androgens in the luteal phase, combined with progesterone, heighten oil output by up to 30%, leading to premenstrual flares characterized by cystic lesions along the jawline.
Estrogen, on the other hand, offers a protective effect by suppressing sebum production and reducing inflammation. Drops in estrogen, such as those during postpartum recovery or perimenopause, can unmask androgen dominance, triggering widespread breakouts. Pregnancy exemplifies this dynamic: early surges in androgens may cause initial flares on the chin and cheeks, while later estrogen rises often improve skin clarity. Progesterone, peaking mid-cycle and in pregnancy, exacerbates oiliness and pore blockage, differing from steady-state acne by its predictable timing. These shifts highlight androgen-driven inflammation as a core mechanism, distinct from bacterial acne driven by constant Propionibacterium acnes overgrowth.
To illustrate the interplay, consider the following comparison of key hormones:
| Hormone | Role in Acne | Common Triggers | Affected Demographics |
|---|---|---|---|
| Androgens | Increase oil production | Menstrual cycle peaks | Women 20-40, PCOS patients |
| Estrogen | Protective, reduces oil | Postpartum, menopause | All adults, especially perimenopausal |
This table underscores how each hormone contributes uniquely to acne development. For example, androgen excess in polycystic ovary syndrome (PCOS) patients often results in persistent, treatment-resistant acne, emphasizing the need for anti-androgen therapies. At NSS Dermatology, recognizing these triggers guides us in recommending options like spironolactone for acne in women with hormonal imbalances. Evidence from clinical studies, such as those in the PMC review, supports that addressing these fluctuations improves outcomes, bridging scientific understanding to practical care.
Identifying Patterns in Adult Hormonal Acne
Adult hormonal acne often presents in recurrent patterns that set it apart from non-hormonal forms, which may stem from diet, stress, or cosmetics without cyclic predictability. Hormonal variants typically manifest as deep, painful cysts and nodules in the lower face, such as the chin, jaw, and neck, rather than the superficial whiteheads of bacterial acne. Our patients frequently report flares aligning with hormonal milestones, allowing for pattern recognition that informs management. For instance, premenstrual acne peaks 7-10 days before menstruation due to progesterone’s influence on sebum, differing from random stress-induced spots by its monthly recurrence.
Postpartum patterns emerge as estrogen plummets after delivery, unbalancing androgens and causing flares that can last months. This contrasts with non-hormonal acne, which lacks such temporal links and responds better to topical antibacterials alone. In perimenopausal women, erratic estrogen fluctuations mimic menstrual flares but with less intensity, often accompanied by dryness from overall hormonal decline. PCOS-related acne shows chronicity without clear cycles, driven by sustained high androgens, leading to hirsutism alongside skin issues. Differentiating these requires tracking breakouts via journals, revealing cycle-induced breakouts that signal the need for endocrine evaluation.
The PMC article on hormonal acne highlights flare predictability, with studies showing 60-70% of women experiencing monthly patterns, underscoring the value of targeted therapies. Non-hormonal acne, per AAD guidelines, involves more widespread pustules without demographic specificity, while hormonal types predominantly affect women aged 20-40. This distinction aids in selecting birth control for acne to stabilize estrogen in cyclical cases, or other hormonal acne treatment like anti-androgens for androgen-dominant patterns.
Understanding these patterns enhances management by predicting flares and preventing scarring. For example, premenstrual patterns benefit from preventive spironolactone, while postpartum ones may require birth control for acne to restore balance. The following table outlines common patterns:
| Aspect | Spironolactone | Birth Control |
|---|---|---|
| Mechanism | Anti-androgen blocks oil | Regulates hormones via estrogen/progestin |
| Timeline | 3-6 months | 1-3 months initial, full 6 |
| Side Effects | Potassium monitoring, dizziness | Mood changes, breakthrough bleeding |
Interpreting this table, premenstrual acne demands cyclical interventions to mitigate predictable sebum spikes, reducing reliance on broad-spectrum antibiotics. Postpartum management focuses on hormonal recovery, with options like birth control for acne offering dual benefits of contraception and skin improvement. At NSS Dermatology, we use these insights to craft personalized plans, ensuring evidence-based approaches that address root causes. By identifying patterns early, patients avoid frustration from mismatched treatments, paving the way for clearer skin and improved quality of life. This scientific foundation directly informs our practical strategies, emphasizing consultation for tailored hormonal acne treatment.
Practical Treatment Strategies
At NSS Dermatology, we recognize that effective hormonal acne treatment requires a multifaceted approach combining daily habits with targeted medical interventions. Patients often seek practical steps to manage symptoms, and we guide them toward sustainable routines that complement professional care. By integrating skincare, lifestyle changes, and prescription options, individuals can achieve clearer skin while minimizing flare-ups.
Daily Skincare and Lifestyle Adjustments
We advise starting with a consistent daily skincare routine to support hormonal acne management. Begin by cleansing twice daily using a gentle, non-comedogenic cleanser to remove excess oil without stripping the skin’s natural barrier. Follow with a lightweight, oil-free moisturizer containing ingredients like niacinamide to calm inflammation and regulate sebum production. Incorporating a salicylic acid or benzoyl peroxide treatment sparingly can help unclog pores, but we recommend patch testing to avoid irritation.
Lifestyle adjustments play a crucial role alongside these topical measures. We suggest adopting a low-glycemic diet, emphasizing whole grains, vegetables, and lean proteins while limiting refined sugars and dairy, which may exacerbate hormonal fluctuations. Regular exercise, aiming for 30 minutes most days, helps balance hormones through stress reduction and improved circulation. Additionally, prioritizing seven to nine hours of sleep nightly supports skin repair and hormonal stability. Tracking menstrual cycles can also reveal patterns, allowing for proactive adjustments.
To illustrate the balance between these approaches, consider the following comparison of lifestyle modifications versus medication-based options. This table highlights key pros and cons to help patients weigh their starting point.
| Approach | Home Care / Lifestyle | Medical Prescription |
|---|---|---|
| Focus | Prevention and overall health | Direct hormone regulation |
| Examples | Diet, sleep, gentle cleansers | Spironolactone, Birth Control |
| Primary Benefit | Low risk, long-term health | High efficacy for cystic cases |
These options are not mutually exclusive; we often recommend combining them for optimal outcomes. For instance, patients who adopt dietary tweaks while using gentle skincare see enhanced results, as supported by clinical guidelines emphasizing holistic care. However, individual responses vary, so consulting our team ensures personalization.
Building on this foundation, we transition to more advanced interventions when basic routines need reinforcement. At NSS Dermatology, our providers assess acne severity to integrate these strategies seamlessly, promoting adherence and efficacy.
Prescription Options like Spironolactone and Birth Control
When hormonal acne persists despite foundational care, prescription therapies like spironolactone for acne and birth control for acne offer targeted relief. We carefully evaluate each patient’s profile to recommend the most suitable option, always emphasizing the need for medical supervision to monitor progress and adjust as needed. These treatments address root causes by modulating androgen activity, which drives excess oil production and inflammation.
Spironolactone, an anti-androgen medication, works by blocking hormones that stimulate oil glands, typically prescribed at 50-200 mg daily. According to American Academy of Dermatology guidelines, it yields about 70% improvement in moderate to severe cases after 3-6 months, though initial purging may occur. Common side effects include fatigue, dizziness, and the need for potassium monitoring, particularly in those with kidney issues. We advise women of childbearing age to use contraception, as it poses risks during pregnancy.
Birth control options, such as anti-androgenic pills like Yaz, regulate hormones through estrogen and progestin combinations. FDA-approved for acne, these can show initial improvements in 1-3 months, with full benefits by six months. They may cause mood changes or breakthrough bleeding, and an initial worsening is possible as the body adjusts. We discuss contraceptive needs during consultations to align skin health with reproductive goals.
Several factors influence the choice between spironolactone and birth control, including patient age, fertility plans, and comorbidities. For women seeking contraception alongside acne relief, hormonal contraceptives often provide dual benefits. Spironolactone suits those avoiding estrogen or needing standalone anti-androgen effects. Shared decision-making ensures the selection fits lifestyle and health history, as evidenced by studies showing comparable efficacy across formulations.
Post-treatment, regular follow-ups at NSS Dermatology allow us to track efficacy and manage any side effects, often combining these with topical therapies for enhanced results. Results vary, and we stress consulting a healthcare professional for diagnosis and treatment. This integrated approach not only clears skin but also empowers patients with lasting strategies.
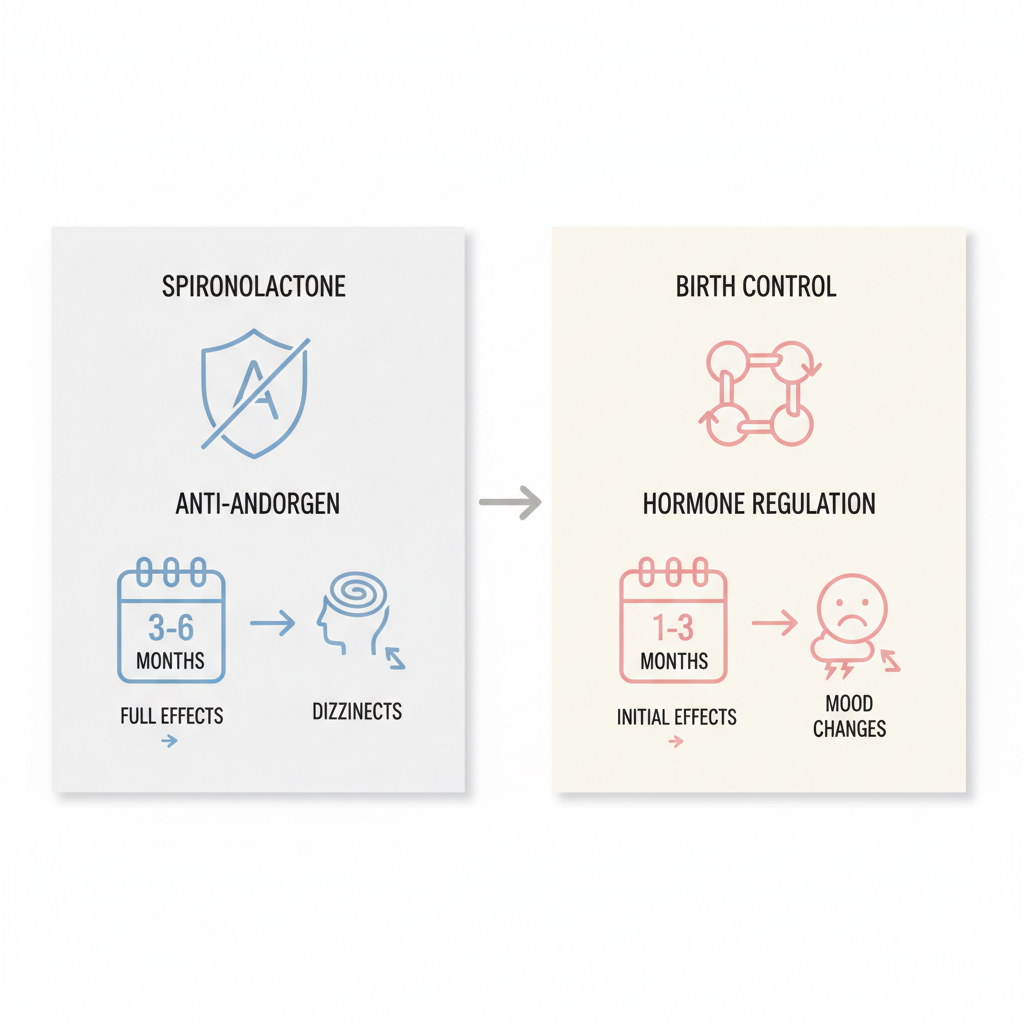
Spironolactone vs. birth control comparison for hormonal acne
In practice, many patients benefit from starting with lifestyle adjustments and escalating to prescriptions as needed. We at NSS Dermatology prioritize evidence-based protocols, drawing from clinical data to tailor plans that minimize risks while maximizing skin health improvements.
Advanced Management Techniques
At NSS Dermatology, we recognize that hormonal acne often requires more than initial interventions for lasting control. Building on foundational treatments, advanced management techniques focus on combination therapies, vigilant monitoring, and personalized escalation to address persistent flares. These strategies integrate hormonal acne treatment approaches, drawing from evidence-based guidelines to minimize recurrence and promote sustained skin health.
We begin with sophisticated combination therapies tailored to hormonal influences. For instance, integrating spironolactone for acne alongside topical agents like retinoids can effectively target androgen-driven sebum production while reducing inflammation. This duo often shows noticeable improvements within three to six months, though full benefits may take longer, emphasizing the need for patience and consistency. Safety profiles are favorable for most patients when monitored, but we always assess individual risks such as potassium levels. Similarly, birth control for acne, particularly progestin-dominant options, offers long-term hormonal stabilization; low-androgen formulations like those containing drospirenone prove effective for many, clearing persistent breakouts over six to twelve months with minimal side effects under supervision.
For severe, refractory cases, we consider extended hormone therapy such as oral isotretinoin, reserved for those not responding to other measures. Lifestyle integration complements these, incorporating stress reduction through mindfulness and a balanced diet low in glycemic index foods to support overall hormone equilibrium.
This comparison underscores the value of transitioning to long-term plans, especially for hormonal acne. According to American Academy of Dermatology guidelines, recurrence rates can reach up to 40% without ongoing maintenance, justifying our emphasis on sustained approaches. At our Midtown Manhattan practice, we personalize these based on patient profiles, ensuring alignment with individual needs and lifestyles.
Monitoring forms the cornerstone of these advanced techniques. Regular follow-ups every three to six months allow us to track progress, adjust dosages, and screen for side effects, fostering extended hormone therapy adherence. We incorporate blood work and skin assessments to maintain safety and efficacy, addressing concerns like the duration of spironolactone effects or optimal birth control selections.
Escalation becomes essential when symptoms persist despite initial efforts. Indicators include deepening scars, widespread involvement, or emotional impact; at that point, we recommend comprehensive evaluations in New York for potential isotretinoin initiation or specialist referrals. Integrating these with our acne treatment services, including Accutane® protocols, supports sustained skin health plans. Consult our board-certified team for evidence-informed guidance, as results may vary and professional evaluation is key to effective management.
Frequently Asked Questions
At NSS Dermatology, we often address common concerns about hormonal acne treatment through patient inquiries. Below, we answer key questions based on evidence from the American Academy of Dermatology (AAD) to guide your understanding.
How long does spironolactone take to work for acne?
Spironolactone for acne typically shows improvement in 3-6 months, as it blocks hormones that trigger oil production. Per AAD guidelines, patience is essential, with full results possibly taking up to a year. We monitor progress closely.
What are the side effects of birth control for acne?
Birth control for acne may cause nausea, headaches, or mood changes initially. The AAD notes these often subside, but serious risks like blood clots are rare. We discuss options tailored to your health profile.
Which birth control is best for hormonal acne?
Combination pills with estrogen and progestin, such as those containing drospirenone, are effective for many. AAD recommends consulting providers, as suitability varies. At our clinic, we evaluate based on your medical history.
How does acne change post-pregnancy?
Pregnancy hormones can flare acne, but it often improves postpartum. If flares persist, AAD suggests resuming treatments like topical therapies. We specialize in safe, personalized postpartum care.
For personalized advice on acne medication queries, schedule a consultation with our board-certified team.
Managing Hormonal Acne Long-Term
Achieving sustained acne control requires addressing hormonal imbalances through targeted treatments like spironolactone for acne and birth control for acne, combined with lifestyle adjustments such as stress management and dietary tweaks to support hormone balance strategies. Ongoing monitoring ensures adjustments for optimal results, as improvements often appear within 2-3 months.
At NSS Dermatology, our board-certified team crafts personalized, evidence-based hormonal acne treatment plans tailored to your needs. We emphasize regular follow-ups to maintain progress and adapt as necessary. Schedule a consultation today to explore these options–contact us at 150 West 55th Street, Suite 1G, New York, NY 10019. As endorsed by the American Academy of Dermatology, hormonal therapies promote long-term success when guided by professionals.
Resources
New York
NY
10019


